We live in an age of health data. Steps, sleep scores, heart rate variability, and VO₂ max. Useful, yes. But if you track only one metric this year, make it blood pressure.
It remains one of the strongest predictors of heart disease and stroke, and it is closely tied to kidney damage and longer-term brain health. The problem is how silent it can be. Many people with high blood pressure feel completely fine while damage builds over the years.
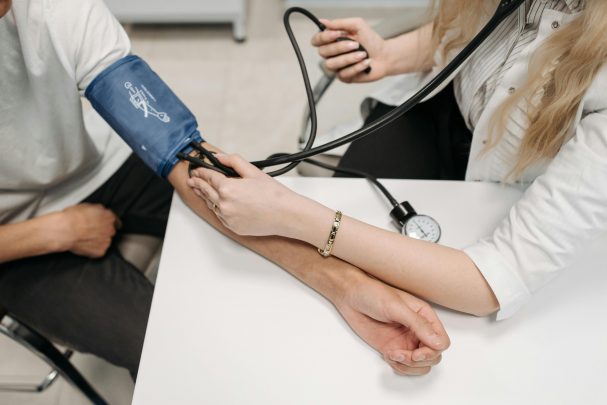
Pexels
Why blood pressure deserves more attention
Every heartbeat pushes blood through your arteries. Blood pressure is the force of that blood against the vessel walls. When the pressure stays too high, arteries stiffen and strain. Over time that raises cardiovascular risk, and it can harm organs that rely on a fine network of blood vessels, including the kidneys and brain.
Even small improvements matter. Large-scale trial analyses show that lowering systolic blood pressure reduces the risk of major cardiovascular events, and the benefit is seen across a wide range of starting blood pressures.
What the numbers actually mean
A blood pressure reading is written as two numbers in mm Hg.
The first is systolic pressure, the peak pressure when the heart contracts. The second is diastolic pressure, the pressure when the heart relaxes between beats.
Common clinical thresholds include normal blood pressure below 120/80 mm Hg, “elevated” systolic 120 to 129 with diastolic below 80, and hypertension from 130/80 mm Hg upward. Some definitions and targets vary by country and by individual risk, so your clinician may personalise what “ideal” looks like for you.

Pexels
Why a wearable is not the same as a reading
Wearables are brilliant for trends like sleep timing, training load and recovery. Blood pressure is different. Most devices do not measure it directly, and estimates are not a substitute for a validated cuff reading. Guidance for home monitoring generally recommends an upper-arm cuff and cautions against finger or wrist devices for accuracy.
How to measure blood pressure at home properly
Accuracy comes from routine. Sit quietly for five minutes first. Keep your back supported, feet flat on the floor, and rest your arm at heart level. Avoid talking while measuring. Take at least two readings one minute apart and record the average. Try not to measure immediately after caffeine, exercise or smoking.
If you are over 40, have a family history of cardiovascular disease, or live with diabetes, kidney disease or known hypertension, home readings can be especially useful to discuss with your GP.
The good news: lifestyle changes can shift the numbers
Blood pressure often responds well to consistent habits, which is where your other “health metrics” can support you.
Regular movement helps. So does building strength alongside cardio. Weight loss, even modest, can make a meaningful difference for many people. Reducing sodium by cutting back on heavily processed foods, and eating more potassium-rich whole foods such as fruit, vegetables and legumes, can help. Sleep matters, too. Poor sleep and untreated sleep apnoea are linked to higher blood pressure. Stress also plays a role, especially if your nervous system is stuck in high alert, which can happen during busy seasons or disrupted routines, including load-shedding schedules that chip away at sleep.
Medication is sometimes necessary, and for many people, the best outcomes come from combining lifestyle changes with the right treatment plan. That is a conversation to have early, not after years of “waiting to see”.
The metric that protects your future self
Blood pressure is not glamorous. It does not come with celebratory notifications. But it is a powerful window into the long-term health of your arteries, heart, kidneys and brain. Track it, understand it, and treat a rising trend as useful information, not a reason to panic.
ALSO SEE:
Featured Image: Pexels

